I know I owe everyone an update post about how BlogHer Entrepreneurs was. (It was amazing.) And I have lovely pics to share from getting to meet two other bloggers IRL this weekend. (They were amazing). And I know I promised on my Facebook page that I’ve got a post brewing about what infertility patients can learn from entrepreneurs. (It will be amazing).
But.
I need to take a break from our regularly scheduled programming to share with you what my husband and I have been slaving over deciphering having late night arguments about working on for the past week as our open enrollment insurance deadline looms large today.
The Backstory
You can get up to speed on the most recent insurance drama here.
It’s pretty short and sweet, really. My husband doesn’t get health insurance through his job, so I have to pick up that tab by making sure my business, Words Empowered*, does offer insurance. I have to because we live in a mandated state, meaning, Massachusetts mandates that every resident must have health insurance.
I don’t pull the small-business owner “we can’t afford health insurance/woe is me!” card because whether we can afford it or not, we need it. It’s good for Massachusetts as a state and it’s good for us.
*For clarity’s sake, everything I do through The Infertility Voice rolls under my business, Words Empowered.
When I originally got health insurance, I signed up with The Cheapest Damn Plan We Could Afford without doing enough homework. As such, we’re now stuck with a $375 RE consultation bill because it wasn’t covered by our Cheapest Damn Plan We Could Afford insurance plan.
Decisions, Decisions
Since it’s Open Enrollment time for us, we get to ditch The Cheapest Damn Plan We Could Afford and now have literally dozens of options. We were torn between two health insurance carriers. For the sake of clarity, we’ll just call them A and B. At one time, my husband used to have insurance through B. They were basically a nightmare to work with.
But (!) they have cheaper deductibles. Here, allow me to illustrate…

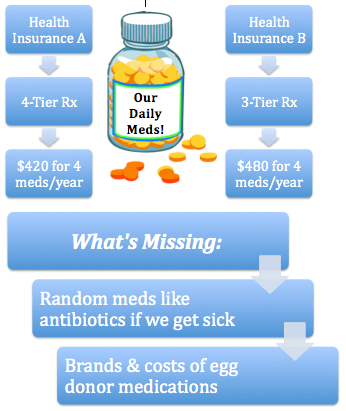
Basically Health Insurance A has higher deductibles than Health Insurance B. In fact, B’s deductibles are HALF of A’s, which is a good thing. Less out of pocket costs for us, right?
But see, there’s this other thing that factors into the equation: our eventual egg donor. Health Insurance A provides coverage for our egg donor’s medications whereas Health Insurance B does not, which means we’d be paying the full cost of those medications out of pocket AND they wouldn’t count toward our out-of-pocket max. At least with Health Insurance A, even though egg donor medications are typically Tiers 3 or 4 (since there aren’t really generic versions of most fertility drugs), we’d still only pay at most a $500 prescription deductible.
Ya follow?
Good, because it’s better than I could earlier this morning.
Egg donor’s medications aside, Larry and I each take 2 daily medications. Both of his are generic (hooray!) and one of mine must be brand (because you should never take generics of thyroid medications; ask me why in the comments). So then we needed to figure out a ballpark range of what it would cost if we just had our four daily meds to worry about.
And then of course, there’s how much we’d have to pay for our health insurance every month. Health Insurance A’s monthly premium is only $840 a month while Health Insurance B’s sits around $810. That $360 difference is nothing to laugh at over the course of a year, either.
So our choices boiled down to the following; do we:
A) Pay $360 more a year for health insurance with higher deductibles and out-of-pocket annual max but dicey prescription coverage if we ever get a Tier 3 or 4 medication (but lower annual costs for our daily medications) that still covers our egg donor’s medications;
OR
B) Pay a lower monthly premium for a plan with deductibles that are half of the other insurance carrier’s plan but risk getting trapped by having no prescription coverage for our egg donor’s medications?
Or, to put it visually:

Or, in even simpler terms…
Six of One, Half a Dozen of the Other
Between fighting off a migraine that started in the wee hours of the morning and trying to anticipate future medical costs between now and April of 2013, it’s a wonder I can even type up a blog post at all because my eyes can barely focus.
And again – this is all in a mandated state where infertility coverage is required by law. Larry and I are not accountants or human resource benefits officers. We’re just two regular people trying to figure out the most affordable way for us to have a family together. The fact that I just had to send ELEVEN forms to the small business association insurance broker to get us all signed up for April 1st coverage is ridiculous.
I know I shouldn’t complain – it’s better that we figure out now what coverage we need than to not have any health insurance coverage at all, right?
And now, it’s time for the “I’m only going to think about this right now and one time only because if I think about it again, I might puke” moment:
I haven’t even factored in what our health care costs become when (not if, because I remain hopeful) we go from two-person monthly premiums to family rates. And that’s all the head space I’m devoting to this sentence because thinking about paying over a grand a month in insurance premiums kind of makes me want to throw up a little in my mouth.
And that hysteroscopy I’m supposed to have done? I honestly can’t tell you how much we’ll be paying for the hysteroscopy right now. And at this point, I don’t have much of a choice. I need to get the procedure done.
I just hope we made the right choice of insurance carriers so we’re not too royally screwed in the end.
All this just so we can build our family.
Correction: all this for just a chance to build our family, because there’s no guarantee that a donor egg cycle would work.
To quote a rather popular movie right now…
May the odds be ever in our favor.

so which did you choose? it really is so very stressful trying to make sure you’ve considered all the variables!!
and I completely understand about the thyroid med situation…on synthroid myself….
Thanks for the information. I wish more people knew what you just wrote and that there are many more people in your shoes (or worse, going barefoot because they can’t afford any insurance). Good luck with your decision!
Ugh. I got a headache just reading that. These decisions are so freaking hard, and in the end, it’s really all a crapshoot, since you just can’t know what’s coming down the road. My two cents, just make a decision and try not to look back, at least not until open enrollment time next year.
May the odds be ever in your favor.
We live in Canada so we have a public health system. Most things outside of fertility based treatments are covered which really sucks because a sex change is covered in our public health system but they cover nothing for infertility. But I digress. We don’t have medical coverage right now until hubby starts working again, but I have yet to find any insurance provider that will cover infertility treatments in any way, shape or form.
We had our appointment earlier this week and they pretty much told us that we have a very small chance of conceiving on our own but if we seek further treatment, IVF is our only way to go and its gonna cost us 12 grand a shot. (or we can moved to IUI with sperm donor with 500 for the procedure plus the cost of the sperm and meds). So now I’m actually looking at getting a second job to help pay for just one shot at this with no guarantee that it will work. I feel your pain hun, though I wouldn’t mind having some coverage, even if its only minimal.
I’m very jealous of your healthcare options and want very much to move to MA so we could have a small business and therefore insurance at a rate like that. We pay about $575 a month for lousy coverage (for the 3 of us, with $25 copays for everything and high deductibles) and only $500 a year in prescription coverage (so I got 2.5 months of my one daily prescription). Zero coverage for anything IVF, let alone drugs to treat infertility which I bet aren’t covered at all even if they cost less than our annual $500 of coverage. Could we be your neighbors? 🙂
Also, tell me more about this thyroid hormone thing. I’m curious!
I want to know about the thyroid hormone thing, too. I’ve been taking generics. We have sucky prescription coverage. I need ammo!
So here’s the scoop on why taking generics for thyroid problems are bad.
By law, a generic must contain the EXACT same formula as the brand name drug when it comes to the active ingredient. That’s the key. A generic can use whatever filler they want to pad out the rest of that formula. Here’s the problem.
Fillers in generics can vary widely not only by generic version, but by batch. When you go to your local CVS and pick up generic levothyroxine, you could be getting one of a dozen or more generic versions. And the generic you pick up one month may not be the same the next month.
So what’s the issue here?
Those generic fillers can actually affect how much active ingredient you’re receiving. So let’s say you take 88mcg. Depending on the generic you receive, you could actually be absorbing 80mcg into your bloodstream. Maybe even as little as 70mcg. Remember, by law, the active ingredient formula must remain consistent. How that active ingredient might interact with the filler, however, is no man’s land.
And then the next month, because generic version B is cheaper, CVS fills your scrip with this cheaper generic who’s filler formula is different that the generic you used last month. Over time, you aren’t getting a consistent dose of the active ingredient, which, we all know is vital to the longterm stability of your thyroid condition.
By getting brand (and it doesn’t matter WHICH name brand, just so long as you stick to one), you’re getting a consistent formula of both active ingredient and filler every time.
If you’re state is anything like mine, your doctor must write “No Substitutions” on every scrip or CVS (or whatever pharmacy you use) is obligated to fill that scrip with a generic. I check my refills EVERY time to make sure it’s brand, because sometimes they screw up.
I used generics for close to 10 years. In the past 3 years, the switch to brand has made a measurable difference in my TSH stability.
So it’s good to know my boss in the pharmacy being militant that we not change generic brands of levothyroxine is reasonable (our usual generic maker has had a low supply of a couple strengths lately)! We stock only one variety of generic and the various brand names that different patients take just for them. So I suppose another answer is read your pharmacist the riot act about no different generic varieties either!
Huh … thanks for this information! I had no idea.
I’ve just had to switch to my husband’s insurance, who now requires I refill my long-term prescriptions by mail. I can only imagine what this conversation is going to be like … !!
Because insurance is mandated, I think it’s generally cheaper. That said, the rate I get for being a small business owner comes at a cost of an additional $225 in annual Chamber of Commerce fees not factored in to the equation here. What really hurts is figuring out that I used to pay $2K a year for insurance when I worked full-time at a major university; now we’re looking at paying over $10K for coverage that’s less than what I got when I had health insurance through my old employer.
Thyroid answer is downthread, under Justine’s comment.
Yikes! I don’t know if it helps, but while the medications for our IVF cycle were pricey, we paid FAR more for the monitoring, the egg retrieval, embryo transfer, cryopreservation, assisted hatching, and ICSI. Those would be my primary concerns for coverage, if I were you (I have no idea how donor egg IVF works with MA mandates, though I’m assuming that all donor procedures and bloodwork must be covered, if you didn’t mention it…)
Thankfully all of that is covered, Drew; basically anything medical for me or the donor. It’s the donor monitoring if done off-site, her fertility meds, and any pre-screening testing, as well as her mental health screen that arent’ covered. And of course, legal fees.